Support from the ground up
Poor quality footwear, exposure to the elements and substandard living conditions can have a ravaging impact on the feet of those experiencing homelessness, but a CBD street podiatry program seeks to address these concerns, and a recent study has shown its positive impact runs even deeper.
Lachie (not his real name) has an acquired brain injury and has experienced homelessness on and off within Melbourne for a number of years.
His injury affects his behaviour and, over the years, has contributed to him being excluded from some support services.
In 2014, the impacts of sleeping rough had a terrible impact on his feet, and at times he was in excruciating pain due to the effects of wounds, callouses and ingrown toenails.
“I had been complaining about my feet being sore. I had corns and they were uncomfortable to walk on – I’d be walking down the street and step on the wrong angle, and I’d yell out in pain,” Lachie said.
“Also, my feet were stinking because my nails were so long. I didn’t know that was the reason they smelled at the time – germs get trapped under the nails … people say your brain controls your body. But your toes control a lot more than you think. You’re always on your toes. And for someone like me, I’m on my feet a lot, walking a lot.”
It was at that time that Lachie, now in his early 50s, first came in contact with Cohealth, a community health service with a centre in the CBD near Queen Victoria Market.
Importantly, he was put into contact with Cohealth outreach podiatrist Rebecca Mannix, who helped Lachie with his several ailments and, importantly, sorting some reliable shoes to help going forward.
“Bec helped me by getting my toes done. And getting me some reliable shoes. She understands the way you walk,” Lachie said.
I had been told to stop walking around so much because I was burning through too many shoes … it’s the only podiatrist I’ve ever used. I’ve never used one before. I wouldn’t know how. Bec has a lot of knowledge about walking on the street. She understands where I’ve been.
Cohealth’s outreach podiatry program is just one of many services it provides to vulnerable people within the CBD and surrounds, and in Lachie’s case it was an important first step.
While podiatry was the first Cohealth service Lachie used, he has since been looped into a range of others to respond to his additional health and social support needs, including allied health and social work.
Having been in and out of rooming houses, Lachie has now been approved for NDIS and is living in stable accommodation.
“Although I’m here to look after his feet, the Cohealth team work together to make sure his holistic health needs are met – social, mental and physical,” Ms Mannix said.
“Lachie has had bad experiences with many services and has been banned for a few due to some of his reactions and behaviours stemming from his brain injury, but we’ve been able to work with him and he comes to see us when he needs something.”
Study confirms essential, “gateway” care
A research paper co-authored by La Trobe University and Cohealth recently published in the Journal of Foot and Ankle Research shed light on the ravaging impacts of homelessness on people’s feet, and the vital role of publicly funded, community podiatry services.
It also found that footcare can be the “gateway” to getting someone connected to other services, such as housing support, addiction treatment and mental health care.
Analysis from the research revealed the most common issues experienced were skin and nail pathologies (68 per cent), biomechanical issues (51 per cent) and acute foot wounds (44 per cent). More than half of people treated by the Cohealth podiatry team had inadequate footwear and nearly one in five required acute wound care.
Overall, Cohealth’s team of specialist podiatrists treat nearly 300 people each year, of which nearly half are people who sleep rough, while one in three are living in unstable housing such as crisis accommodation and rooming houses.
“When you’re sleeping rough or cycling through rooming houses it’s hard to keep feet clean and dry. People often don’t have access to basic podiatric items such as clippers, and problems snowball quickly,” Ms Mannix said.
“Having flexible, adaptable services that are designed with clients is really important so that they get the healthcare they need quickly and not wait until problems become emergencies.”
Community-based podiatry services that use an outreach model are vital to improving the overall health of people who are without a secure home, according to Cohealth.
“Without our podiatry service and outreach model, a great many of our clients would suffer with painful feet, whilst their feet are their only way of getting around,” Ms Mannix said.
“A key feature of the community health model is that we can help people with other issues beyond the service they may be presenting for. Everyone has the right to live free of pain, and to have access to high-quality health care.” •
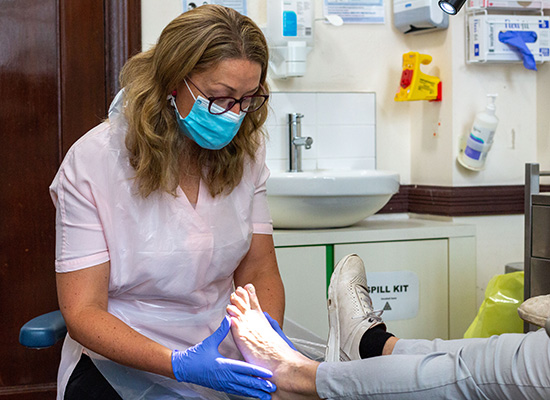
Caption: Outreach podiatrist Rebecca Mannix treating a patient at Cohealth’s CBD community health centre (Picture: Will Hawke).

Council backs AI push, framing moment as Melbourne’s “fork in the road”








 Download the Latest Edition
Download the Latest Edition